|
After the failure to achieve LBBP, we returned to mapping the HB region, in search of a better pacing threshold. Some maneuvers were done to let lead jump across the mid-myocardial scar and fall into LBB area like giving rapid turns with some force on the sheath but were not successful. Challenge was predominantly reaching mid-myocardial. In view of the possibility of tissue in helix of lead, it was cleaned of tissue bites after every attempt. Up to four sites including a distal part of septum were tried but lead did not advance beyond the initial one or two turns. Keeping in view the possibility of basal septal scar, posterior fascicle pacing was attempted by targeting the mid and posterior septum. The C315 sheath was positioned along the interventricular septum, 1–1.5 cm below the HB position but the lead could not be screwed into the left bundle as there was reverse transfer of the torque. The C315 sheath was advanced over the Teflon wire into the apex of right ventricle (RV) in right anterior oblique (RAO) projection along an imaginary line between the His bundle (HB) and RV apex using a road map of initial position of HB. Therefore LBBP was considered alternative and was attempted. Distal His position was tried but the threshold remained high (Fig. 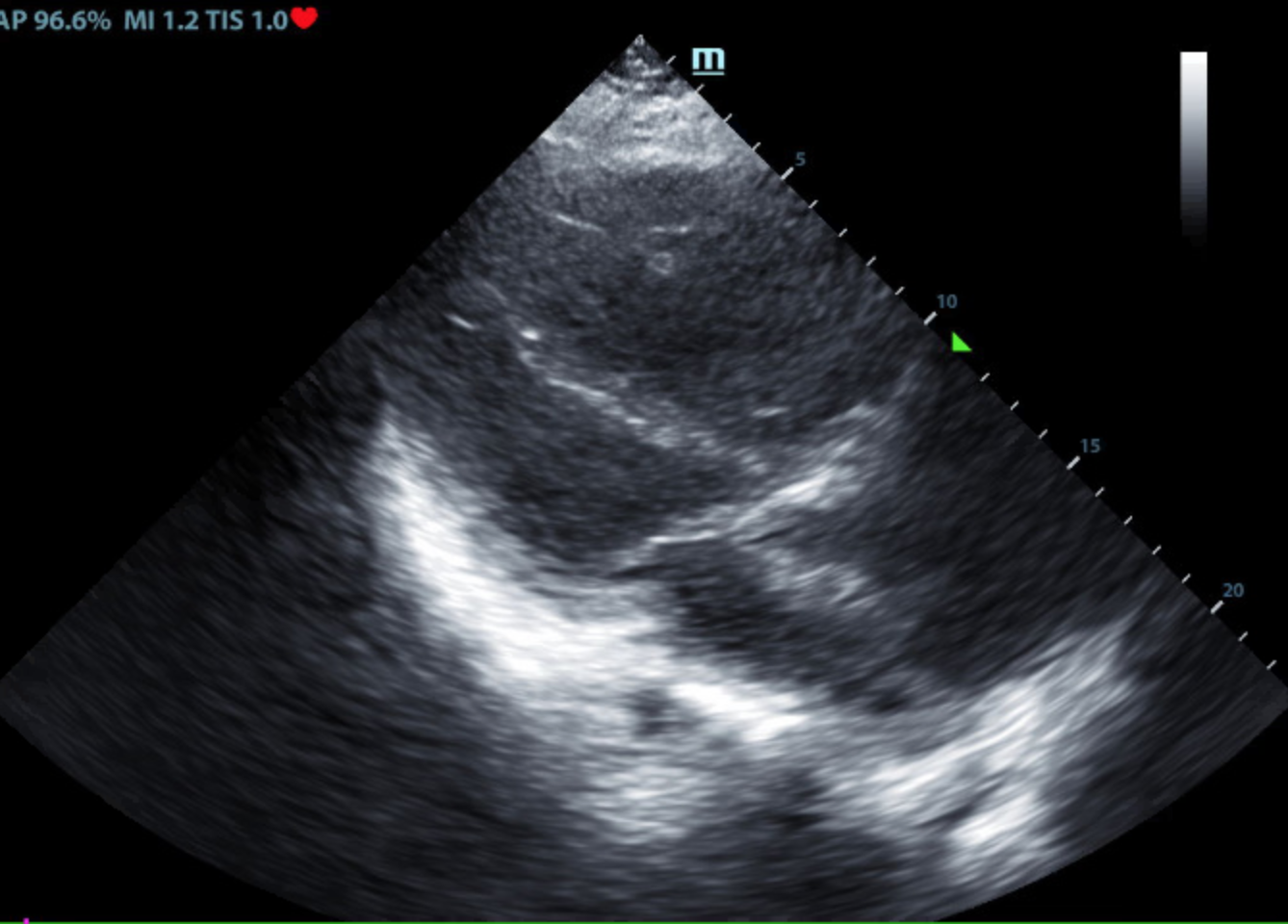 
Pacing was done 5V 1 ms, resulting in nonselective HBP pacing. Local EGM showed His bundle potential in unipolar configuration. C315 catheter was pulled back into right atrium (RA) and turned anticlockwise to align it along the upper tricuspid annulus/RA junction. The lead was connected to Workmate Claris EP system for intracardiac electrogram (EGM). The Select Secure lumen less 4.1-F sized, 69-cm length 3830 SelectSecureTM active pacing lead (Medtronic Inc., Minneapolis, MN) was taken into the sheath. A fixed-curve sheath (C315 His, Medtronic Inc., Minneapolis, MN) was advanced over long Teflon wire into the right ventricle (RV). The previous device was removed and the old leads parameters checked and secured. A slippery Terumo wire was passed through the venous narrowing and access secured. A fluoroscopy-guided left subclavian access was obtained using Seldinger technique. A significant narrowing at left brachiocephalic and superior vena cava (SVC) junction was seen (Fig. Atypical left bundle branch morphology defined as QS or rS in lead V1, broad R waves in lead I, and aVL but with QS or rS in V5-V6 is associated with favorable echocardiographic response to CRT and displays similar survival rates to typical LBBB patients.Ītypical left bundle branch block Cardiac resynchronization therapy Heart failure Left bundle branch block.A left axillary/subclavian venogram was taken from peripheral access vein to confirm patency. This subgroup of IVCD should be considered for CRT. Patients with ALBBB may have a favorable echocardiographic response to CRT and display similar survival rates to typical LBBB. Cumulative 2-year survival was 88% in ALBBB, 86% in TLBBB, and 76% in OIVCD (p value = 0.011). A multivariable model showed a lower likelihood of echocardiographic response in OIVCD and a similar likelihood in ALBBBB compared to TLBBB. 75% and 72%, respectively, p = 0.01 for both comparisons).  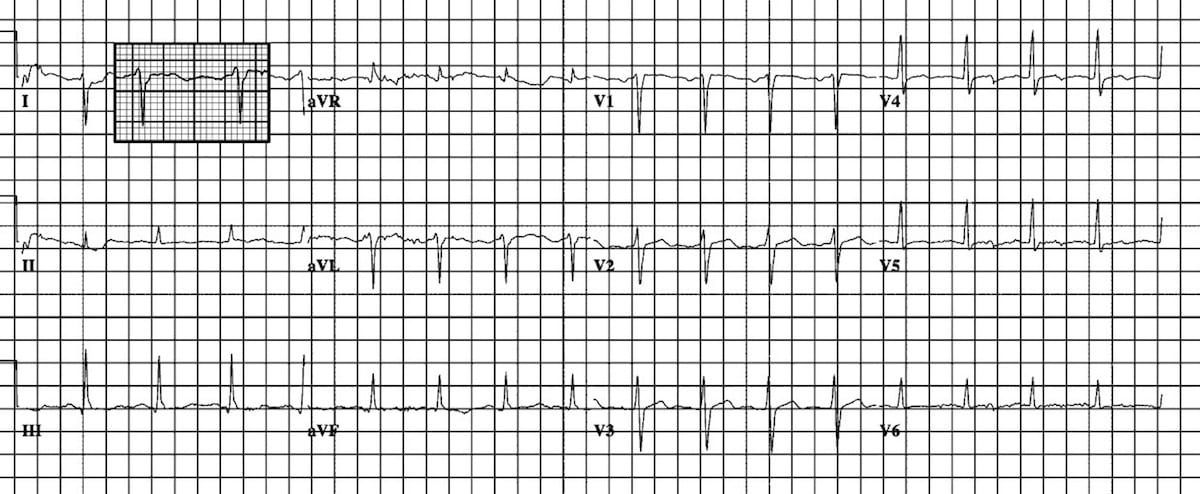
Rates of echocardiographic response were lower among those with OIVCD compared to those with LBBB and ALBBB (50% vs. Endpoints were 2 years mortality and echocardiographic response, defined as a decrease of ≥ 10% in indexed LVESV or an increase of ≥ 5% in left ventricular ejection fraction at 1 year of follow-up.īaseline clinical characteristics were similar among all the three groups. ECGs were classified into the following three groups: (a) typical LBBB (TLBBB) according to accepted guidelines (n = 67) (b) IVCD with LBBB pattern criteria in V1, 1, and aVL but with QS or rS in V5-V6 which we defined as atypical LBBB (ALBBB) (n = 74) and (c) all other IVCD (OIVCD) patterns (n = 98). However, IVCD pattern is heterogeneous, and it is possible that QRS patterns may also respond to CRT.Ĭonsecutive baseline ECGs of 239 patients implanted between 20 with CRT were analyzed. Response to cardiac resynchronization therapy (CRT) is well-established in patients with typical left bundle branch block (LBBB) but modest or even negative in those with intraventricular conduction delay (IVCD).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
